A Day in Asahan
Team EMAS in Asahan
Neonatologist Dr. Jeff Bartlett from Children’s Hospital Connecticut works with Save the Children’s Dr. Wilson Wang and the rest of the EMAS clinical team to improve the care of newborns at HAMS Public Hospital in Asahan District, Indonesia. HAMS may be only one of over fifty hospitals that EMAS currently supports, but its strength as a health facility is as important as any other. For many poor sick patients in the district, HAMS Hospital is the last resort health facility. The roll out of the nation's new national health insurance program BPJS earlier this year means HAMS has further potential to test the relationship between patient access to care and quality of care.
It is the first time that Dr. Bartlett has been to Indonesia let alone worked abroad as a neonatologist. He is part of a unique Save the Children-Boston Children’s Hospital Collaborative, which places pediatricians for up to a month in select hospitals supported by EMAS, a USAID funded program targeting neonatal death in Indonesia, among the highest in Asia. Whether in Indonesia, Liberia or the United States, newborn survival means support of a discrete set of interventions, namely excellent resuscitation of apneic newborns, appropriate feeding of low birth weight infants and stabilization and treatment of emergencies including profound infection, dehydration and respiratory distress. Twelve American pediatricians have worked with EMAS doctors, staff and partners this year.
On this mid-June morning, the care team consisting of head neonatal nurse Zulismar, vice nurse Ibu Aurora, EMAS quality improvement coordinator Flo Ridayu, Wang and Bartlett is interrupted by the arrival of a three day old who has stopped breathing. The team had been discussing progress on weight gain of patients using new EMAS feeding tools, on associated quick weaning of the babies from intravenous fluids and on the plan for the day which included review of neonatal resuscitation and its proper documentation.
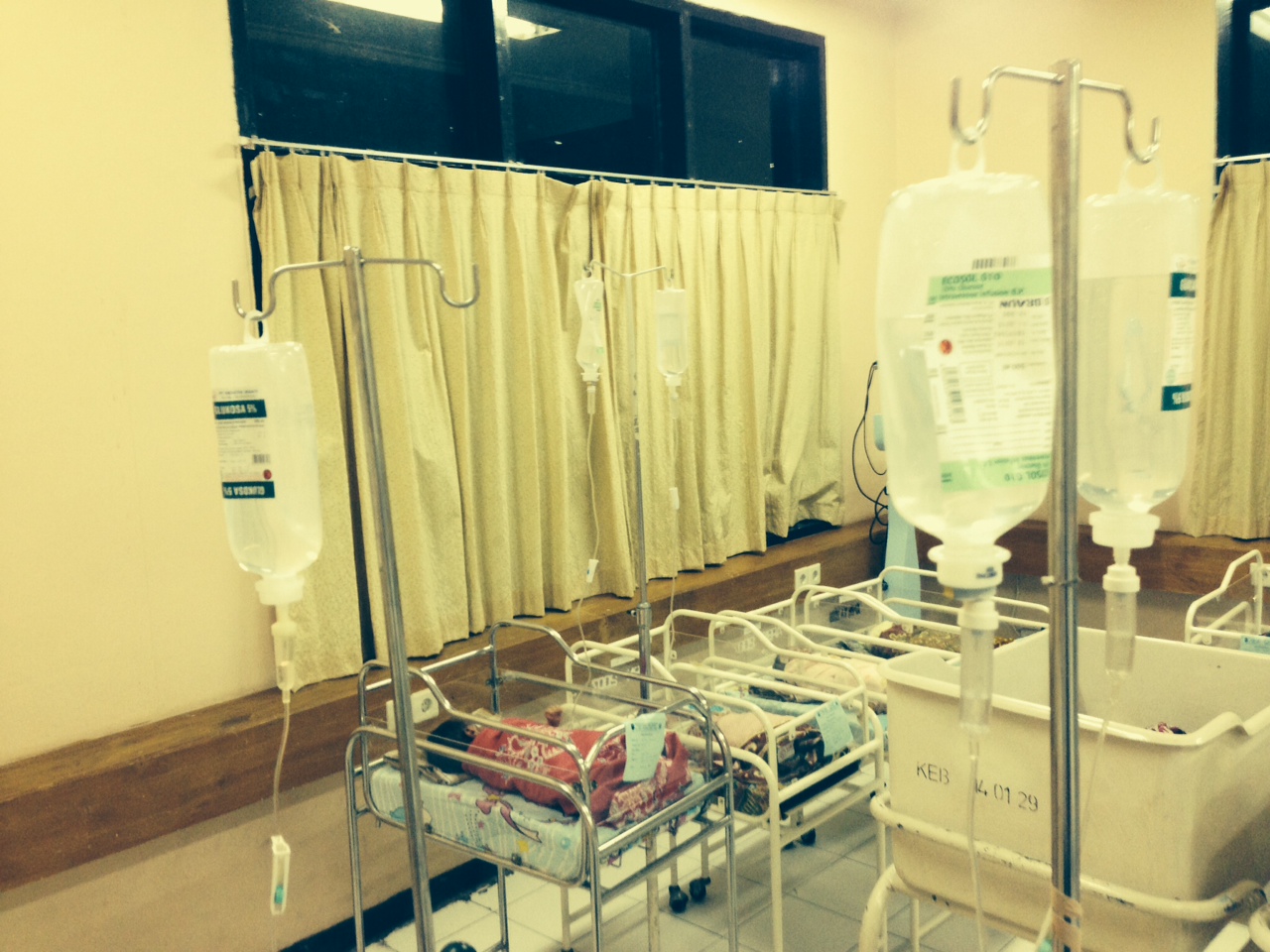
Baby with life threatening sepsis. Note, petechiae forming on lower abdomen.
While Nurse Zulisman places an intravenous line in the baby’s foot, Dr. Bartlett confirms a heart-beat less than sixty beats per minute and begins positive pressure ventilation with a bag valve mask from a well-stocked emergency trolley—one of many system level interventions organized under EMAS. Dr. Wang meanwhile gathers the baby’s medical history that can inform more accurate treatment. The baby like too many had passed through the medical system without any accompanying documentation—a paper with only the referral center’s letter-head and the patient’s name.
Before finding the baby’s caregiver, Dr. Wang pauses to invite the ten or so medical students who are waiting for attention outside the unit as they are every day. Dr. Wang twenty years later still remembers what it felt like to be a simultaneously eager, frustrated, excited and ignored medical student. He decides that these future doctors must learn from this case, whatever the outcome.
The parents are coming and the unit’s pediatrician is on the way. Dr. Wang speaks with the mid-wife who has transported the three day old from the neighboring “Puskesmas” or health center. After fifteen months in Indonesia, Dr. Wang speaks semi-fluent Indonesian but still Flo has to occasionally fill-in the gaps. He is acutely aware of the balance between him modeling behavior for others and him taking away responsibility from others. Perhaps this time he balances the wrong way. It’s hard to tell, because there is a baby to his left with life threatening bradypnea and bradycardia, the doctor in the unit has yet to arrive and at least fifteen or so medical students and nurses and support staff await to see what they as a team will do. This could be the most important lesson.
The baby was born small at 2300 grams but was active and without issues on discharge to home. The midwife had actually delivered the baby in the Puskesmas instead of her home at the behest of the District Health Office, which was increasingly pushing in-facility births. But the next morning, the mother had called her in a panic describing the baby as choking on its breast feeds. At the Puskesmas the baby was thought to be lethargic so he received oxygen. The nurse urged the patients to go to Asahan’s District Hospital but the baby had yet to be enrolled in BPJS and the parents feared an exorbitant medical bill. The baby remained below conscious and sick. Sure enough, early the next morning when the mother attempted breast-feeding, the baby apparently choked and changed color again. The mid-wife explained to the parents that this was aspiration and that they had best go to the hospital at whatever the cost. She told them that she would take the baby herself to make things quicker and that the parents were to follow immediately behind
80% of diagnosis is in the history. Without complete and organized notes, doctors receiving sick patients often work in the blind.
With such a history, the diagnosis is actually acute life threatening event (now called BRUE), which Dr. Bartlett explains to Flo, Zulisman and the medical students. Aspiration would present as fast breathing and this baby is unfortunately not breathing at all. Also, newborn babies rarely aspirate at the breast as they are able to control flow with suck and a mother’s milk volume in the first few days is scant— on the order of drops.
Acute life threatening event, on the other hand, is defined as any condition in which the parents believe their child’s life is threatened. Whatever the semantics, the parents of this baby were right. No less than five minutes after the start of resuscitation, Dr. Bartlett notices small red dots, or petechiae, spreading across the baby’s lower abdomen. This is a clinical sign of blood escaping the capillaries into the skin in response to bacteria in the circulatory system. The blood pressure drops. So now the diagnosis is changed from acute life threatening event to disseminated intravascular coagulation resulting from bacterial sepsis—the second leading killer of newborns in the world.
By this time the pediatrician covering Asahan’s perinatal unit, Dr. Tuti, has arrived. Wang quickly explains the patient’s history and asks her if she might do anything differently. She says “tidak”, thanks the team and asks them to proceed. With the appearance of the petechaie, Bartlett has Zulismar give the baby ampicillin and gentamicin. Wang and Bartlett would later discuss that they should have given antibiotics before the appearance of the petechaie. Better yet, the health center should have administered antibiotics before transfer to Asahan four hours ago. The oversight at both levels, however short at Asahan, nevertheless represents a vital delay in care and reminds the team yet again of the importance of clinical checklists to support decisions made in high stress environments. SAVE has been experimenting with scientific medical protocols—those usually found in large dusty notebooks-- engineered into the normal clinical work flow to make them convenient and useful. So for this baby, instead of the medical staff using simple recall to treat its many conditions, the nurses and doctors could have followed a form that listed out the most important considerations such as testing for blood sugar, administering Normal Saline at 10cc/kg and giving ampicillin at 100mg/kg and gentamicin at 4mg/kg. This dying baby via the presence of Wang and Bartlett, Zulismar and and now HAMS pediatrician may well be receiving the most specialized attention of any baby in the country and yet simple vital behaviors listed on a medical emergency check list would have similarly and even more effectively improved its care.
What Dr. Wang does not miss is the type of fluid hung on the IV pole, dextrose 10%. It is the standard fluid used for babies in the unit but the choice of fluid in this case is wrong. Wang explains to Zulisman that nutritive fluids must always be distinguished from resuscitation fluid. Zulisman quickly changes the fluid to normal saline with a nod. She asks at what rate and Dr. Wang laughs because the math is so complicated. The unit doesn’t have an infusion pump so liquid is dispensed through the line with only gravity as the pull. In this way, 60 drops of fluid represents a single milliliter of fluid and the baby needs 10 milliliters of fluid per kilogram of weight. Dispensed over 30 minutes this is... Wang asks the medical students to do the calculation after he explains the details of the calculation one more time. He comments, “kadang kadang, memang, teknologi penting…In some cases technology does help.”
One hour goes by. The baby has been resuscitated with appropriate fluids. The baby has received antibiotics. The blood sugar of the baby is high enough. Yet, whenever the team stops breathing for the baby, the baby’s heart slows. The baby also has yet to move save for the one time Dr. Wang saw the baby open his eyes to look at him, gaze wistfully to the left only to close them again. In retrospect Wang is not confident. Was this a clinician’s mirage? Dr. Bartlett suggests stopping resuscitation. Dr. Wang after looking at the babies pupils and seeing that they are still reactive—a true sign of life-- he suggests giving the baby a little more time.
Medical students practicing real care
In the United States, this baby would simply be connected to a ventilator but Asahan District public hospital does not have a ventilator. After a short strategy session, Dr. Wang and Bartlett begin teaching the medical students proper bag valve mask technique and concomitantly how to empty the stomach of air that accumulates from the ventilation process. Without this, the stomach will balloon into the pulmonary space making it difficult to breathe for the baby. They establish a conveyer belt like system of medical students. S/he who has the undesirable task of emptying the stomach of air then goes to do the bag valve mask. Those who just finished the bag valve mask act as technical advisors to those just taking on the job. After a few rounds, the medical students are prepared to be independent. Dr. Wang says in Indonesian, you are the baby’s ventilator. You are buying time for a miracle to happen. We will do this for an hour and then reassess. “Setuju?” Agreed reply the students, “Setuju.”
Wang, Bartlett, and Zulisman move to the other room to continue focus on strengthening the routine care of infants. They are not casual in their departure but are following a pattern characteristic of international medicine: You multi-task between simultaneously vital events. Wang is convinced that by standardizing the everyday care of newborns at HAMS, they will actually prevent many more deaths than the type occurring in the adjacent room. When the team first arrived, they noticed that patient vital signs were only intermittently and inconsistently taken. The nurses weighed babies on the floor on a manual inaccurate scale. All of the babies were being fed insufficiently with average weight loss of the babies less than 7 days of age exceeding the normal range by over 30%. Babies who should have been gaining 20-30 grams per kilogram per day were gaining an average of 1 gram per day, a startling dangerous figure.
It's all about the homework. Amazing Zulismar and Aurora